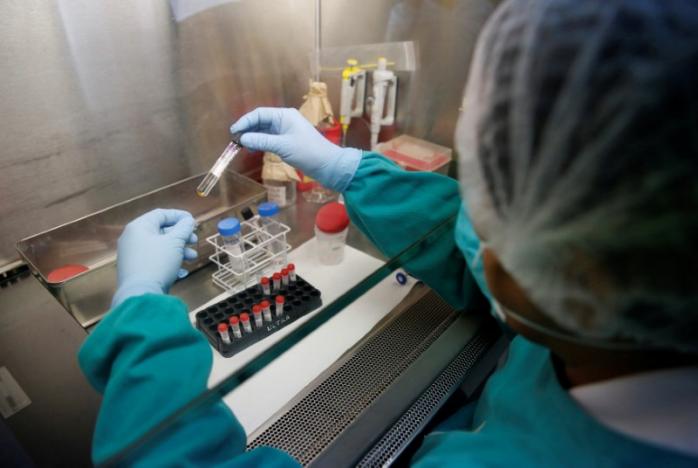
Bloody hell! Transfusion happening without testing blood for deadly diseases
- THT EXCLUSIVE
Infected persons with negative reports during window period may donate blood
- Dr Anup Bastola, Consultant Tropical Medicine Physician/HIV
Kathmandu, June 13
As the world marks World Blood Donors’ Day on June 14, a teenager in Kathmandu is living with Human Immunodeficiency Virus. It is suspected that the teen got infected during blood transfusion and tested positive on May 7.
“Suffering from a blood related disease, the teenager has been getting regular blood transfusion since early childhood,” a family member told THT. There is no family history of HIV. The patient is neither sexually active nor into drugs,” Consultant Tropical Medicine Physician/HIV Dr Anup Bastola told this correspondent.
Clinician at Sukraraj Tropical and Infectious Disease Hospital, Teku, who is also looking after the patient, pointed to blood transfusion as the mode of infection.
Urmila (name changed on request) is another resident of the capital who has contracted HIV through blood transfusion. A patient of aplastic anaemia, she has been dependent on blood transfusions since 1993. She tested positive for HIV five years ago. “I am sure I got the virus from blood transfusion, as I never had sexual relations with anyone other than my husband. My husband is not HIV-positive, neither are our children,” Urmila told THT.
Though National Centre for AIDS and STD Control has no record of the first HIV case diagnosed from blood/organ recipients, it is estimated that by September 2007 24 such cases had been reported.
According to NCASC, since July 2016, 116 people have contracted HIV due to transfusion of blood and blood products — 78 males, 35 females and three transgenders. This figure is 0.4 per cent of the total 28,865 HIV cases in Nepal. Majority of such cases were reported from Kathmandu, Palpa, Sunsari and Jhapa districts.
There are 105 blood transfusion service centres in the country, with National Public Health Laboratory, Teku, responsible for ensuring quality of donated blood. The blood needed for medical purposes is usually collected at blood donation camps.
“The collected blood should be tested for Hepatitis B, Hepatitis C, HIV and Syphilis,” NPHL Director Dr Raj Kumar Mahato told THT. He added that though different tests and screenings are done there is no testing kit for the window period testing of HIV in the country.
“If a person is infected with HIV, the antibodies in his/her body become active only after three months of the infection,” informed Dr Bastola. Only a special test — Nucleic Acid Amplification Test — can detect HIV/HCV (Hepatitis C) in blood during this window period. But due to unavailability of test kit in Nepal, there is risk of HIV infections through blood transfusion, as infected persons with negative reports during window period may donate blood,” said Dr Bastola.
“NAAT can detect HIV after 10-12 days of infection during the window period. It is also helpful for testing Hepatitis B and C,” said Dr Mahato.
“We try our best to provide safe blood to patients through our rapid test and enzyme-linked immunosorbent assay (ELISA) test. These tests are used to determine whether blood has antibodies related to certain infectious conditions.
However, there isn’t any kit to detect HIV in its window period in the country. People receiving blood at times can get infected with HIV. But it’s very rare,” claimed Ram Shrestha, programme officer at Central Blood Transfusion Service, Nepal Red Cross Society, Balkumari.
Besides NAAT, other tests to detect Human T-lymphotropic virus -1 and HTLV-2 that cause leukaemia and myelopathy of the spinal cord are also not available in the country.
“They aren’t tested as they aren’t in the Blood Transfusion Guidelines,” informed Dr Manita Rajkarnikar Shrestha, director, CBTS, NRCS. “If these are made mandatory, we’ll
conduct the tests.”
“NAAT is very expensive. It costs around Rs 68,000 per test,” said Dr Rekha Manandhar Shrestha, consultant pathologist, NPHL,and co-ordinator, National Bureau for Blood Transfusion Service.
“The HIV cases from blood transfusion are comparatively low compared to other modes of transmission. We have limited resources to meet all groups and we haven’t done anything till now for blood/organ recipients,” Bir Bahadur Rawal, strategic information officer at NCASC, told THT.
So what should be done to mitigate the risk of HIV transmission through blood? Dr Manandhar Shrestha says donors should be aware about their health before they donate blood.
But asking donors to be aware is obviously not the solution. Until authorities concerned take a more serious stance on this issue, there is little hope for Urmilas in Nepal.