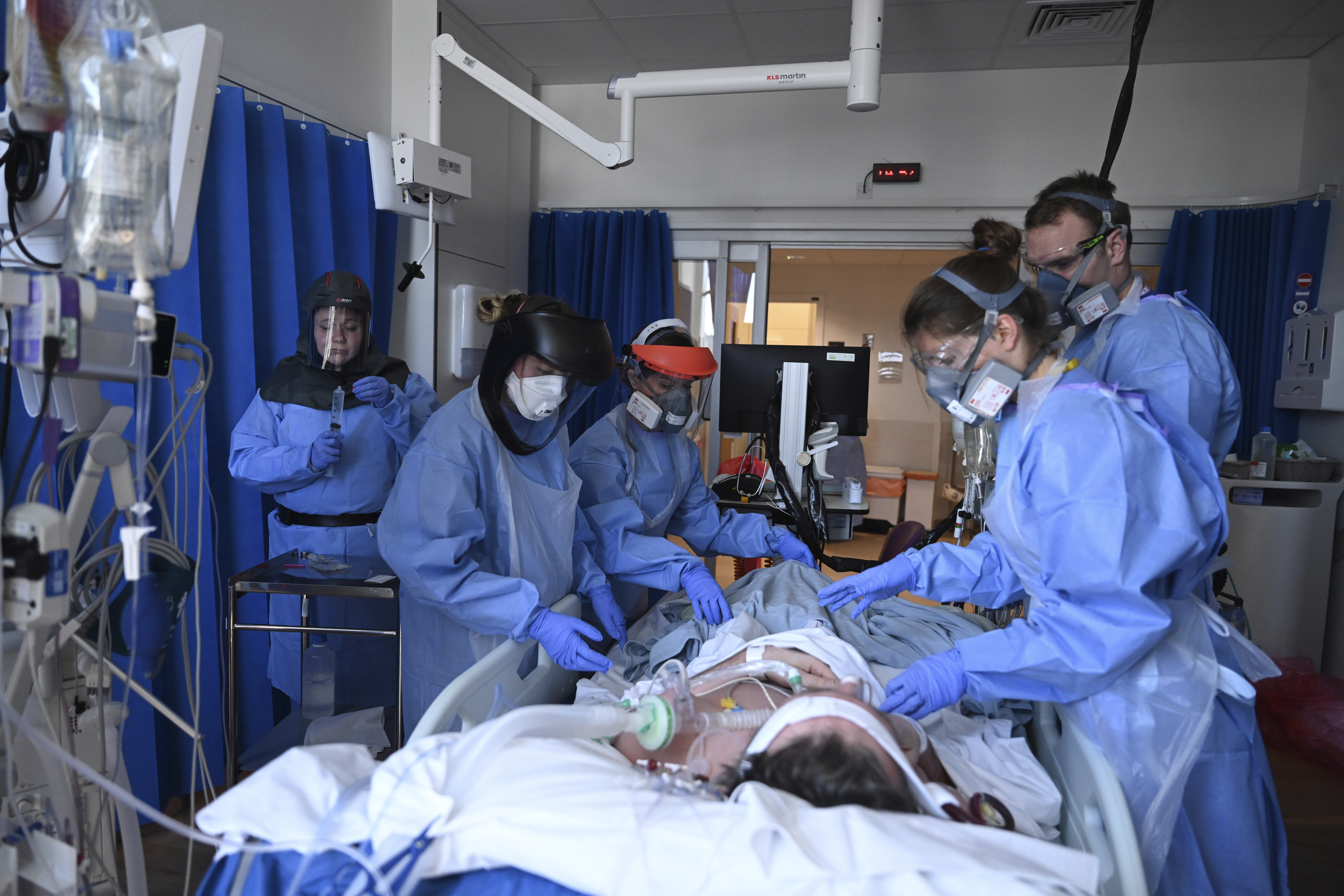
Problems of medical professional service
May 20, 2020
Chirayu Lekhak
A young aspiring student dreams of becoming a medical professional with the hope that he will someday selflessly serve the needy and the poor. He does well in his studies, passes his entrance examination by putting extraordinary amount of hard work and perseverance, all just to lose a seat to a less deserving candidate on the basis of reservation: Nevertheless he doesn’t give up on his dream. He continues to try, gets into a college, completes his study amidst all the ragging and gets his license approved. He works tirelessly, usually more than a hundred hours a week, providing selfless service for very minimal pay!
As COVID-19 runs rampant, he uses all his acquired skills and knowledge to protect himself and others. After a long day and night of duty, he wants to return home but is stopped from entering the house by his landlord because he who has been helping everyone get better will infect the landlord and his family. More than a decade of study and tireless practice and in the end becomes a victim of discrimination and violence by the very people he pledged to serve and do no harm in any circumstance. This is a sad story of many physicians and medical workers in Nepal and also south Asia as a whole.
Being a doctor is an occupational service requiring special training in different sections of science. It requires holding a professional license achieved through long strenuous hard work and effort. Doctors are often held in very high esteem in almost all parts of the world. But no physician, however conscientious or careful, can tell what day or hour he will be the object of some undeserved attack, malicious accusation, blackmail or damage suit.
About a decade ago, violence against doctors or other medical fraternities hardly made any news, or hardly was a matter of discussion in Nepal as it was very infrequent, though such violence in western countries was already known. Very often, such abuse of the medical professional was caused by the patients themselves, who were under the influence of alcohol or drugs and were delirious or were in the psychiatry ward.
However, in the context of south Asia, including Nepal, violence against doctors shows a different picture. More often in Nepal, the patients themselves are not the violence makers but their relatives. This is out of emotion. Anxiety, long waiting period before the patient can speak to a doctor and the feeling that the doctor is not giving enough attention to his/her patients engender frustration, giving rise to violence. Bereavement, a young patient under serious condition, only earning member in the family and only child with serious disease evolve emotional outbursts, which may quickly end in violence. But violence against medical workers, who have been working all their life for the welfare of the health of others, cannot be justified.
Violence against a junior doctor in West Bengal, India triggered a series of events, which made it possible for the central government of India to pass the Medical Protection Act to ensure the safety of doctors across India. The nationwide fraternity of doctors had shown tremendous support by staging protests and withdrawal of all non-emergency services like OPD. Violence against doctors and medical workers has been increasing in Nepal, but no specific law has yet been set up in order to protect the medical workers and their working environment.
Patients, their relatives and society at large hold immense responsibility to prevent such violence. A dispute between patients and hospitals or doctors is not to be sorted out through violence, but in a civilised society, through dialogue and rule of law. A democratic system addresses any ill doing by the rule of law, and no one, whether a patient or doctor for that matter, is above the law.
What the society needs to understand today is that being a doctor is not solely a service, it is also one’s profession; thus it is considered professional service. It is the tertiary sector of the world economy. During such a pandemic, the need of doctors has been more than realised everywhere. Being a doctor, without doubt, is tough and tiring, but this service provides both mental and emotional satisfaction. But when a doctor or working intern for that matter is forced to work for more than 30 hours in a stretch, he cannot achieve work satisfaction and also fails to deliver quality of work the profession demands and requires.
The allocated budget of Nepal for the health sector and insurance is very low, and more than 50 per cent of it accounts for funds provided by international aid. This fails to provide sufficient facilities in the hospitals and healthcare centres and also fails to provide proper services to the medical workers. Working in an environment with poor facilities has been a long-standing problem that physicians in Nepal face, and despite the aid by rich donors, it will continue to be a problem until the government works in unison and transparency with the related medical authorities.
Rich private hospitals have more facilities than the government-funded healthcare facilities, thus very few can afford to pay for the treatment costs in Nepal. To live a healthy life and get proper healthcare is a fundamental right of all, irrespective of one’s wealth and stature.
There are other existing long-term problems in our health sector like the doctor-population ratio and lack of quality medical workers. Recent statistics put the total number of doctor in Nepal at 16,432, with a doctor to population ratio for the whole country standing at 1:1724. The primary reason for it can be traced to the expense needed for the study. Although many scholarships are provided by the government, the system of reservation rather than meritocracy at every step demotes the quality of production of professionals.
These problems will only continue to grow until proper action is taken by the government. Only by ensuring safety and quality of medical workers can a country expect the safety of its citizen.
Lekhak is an intern at the First Hospital of China Medical University (CMU), China